Table of Contents
Knee pain that persists can begin to affect how you move through your day. You may hesitate before simple movements, unsure how your knee will respond. As discomfort or a catching sensation develops, even routine activity can start to feel unpredictable.
These symptoms can be caused by osteochondritis dissecans (OCD). In some cases, joint irritation may also lead to inflammation similar to knee synovitis.
At Resilience Orthopedics in Los Gatos, we focus on identifying the source of your cartilage injury and creating a treatment plan to help you move comfortably again.
Book a Consultation with Dr. Pamela Mehta, MD
The Best Orthopedic Surgeon in San Jose
Dr. Mehta is a board-certified orthopedic surgeon who can help you recover from your joint condition. If you:
- Are Suffering From Pain and Mobility Issues
- Need Orthopedic Assessment and Advice
- Want Treatment From a Top Orthopedic Doctor
We Can Help
What is Osteochondritis Dissecans?
Osteochondritis dissecans is a condition in which a small area of bone and cartilage loses blood supply and begins to weaken. It affects the knee, especially in active individuals and young athletes.
As the condition progresses, the weakened area can lead to symptoms such as locking or catching. In more advanced cases, the fragment may loosen and become a free body within the joint.
[Image showing the knee joint with a loosened cartilage fragment.]
OCD can develop from repetitive stress, a direct injury, or underlying factors such as genetics or reduced blood flow. Symptoms may include:
- Knee pain that worsens with activity
- Swelling or stiffness
- Locking or catching sensations
- Limited range of motion
- A sense of instability when moving

When to Seek Urgent Evaluation
While osteochondritis dissecans often develops gradually, certain symptoms suggest the joint may be under more immediate stress and should be evaluated promptly:
- Sudden knee locking that prevents full bending or straightening
- Persistent catching sensations that do not resolve
- Swelling or pain after a twist or impact
- The knee gives way or feels unstable
When these symptoms appear, early evaluation can help prevent further joint damage and guide appropriate treatment.
How We Treat Osteochondritis Dissecans at Resilience Orthopedics
At Resilience Orthopedics, we identify the cause of your symptoms and create a treatment plan tailored to your activity level and goals.
Diagnose at Resilience Orthopedics
We begin with a detailed review of your symptoms, activity level, and medical history. This helps us understand how your knee is functioning in daily life.
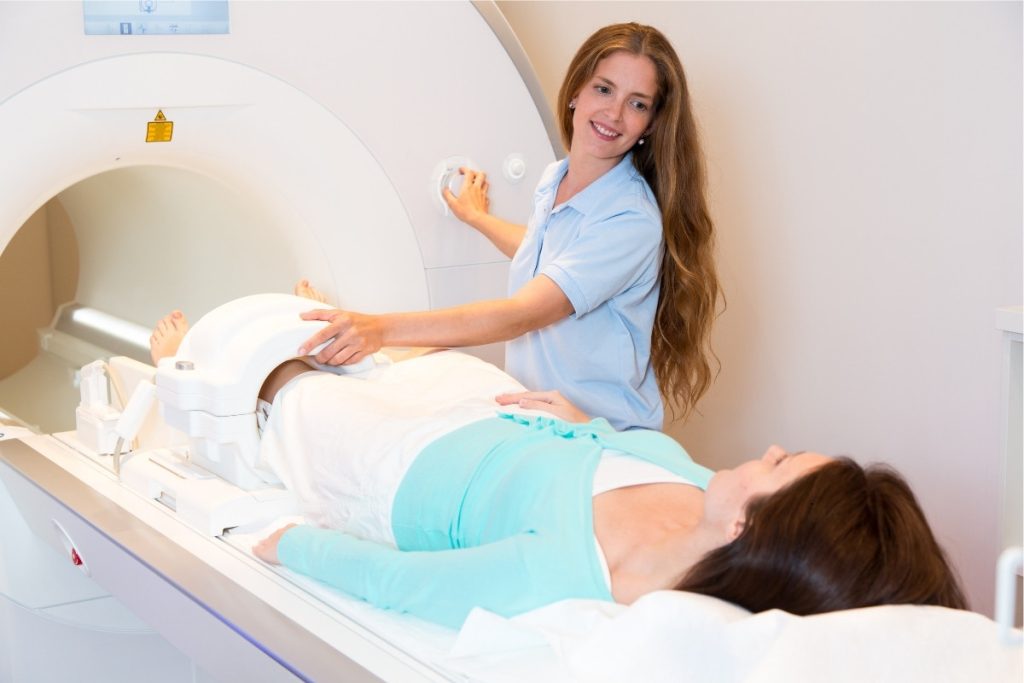
Evaluation may include:
- Physical examination to assess motion and stability
- X-rays (included at your first visit unless recent imaging is available)
- MRI to evaluate cartilage injury and lesion stability
How Do We Treat Osteochondritis Dissecans?
Most cases improve without surgery. Treatment focuses on reducing symptoms, protecting the joint, and restoring function over time.
This may include:
- Activity modification to reduce stress on the knee
- Anti-inflammatory medication for pain and swelling
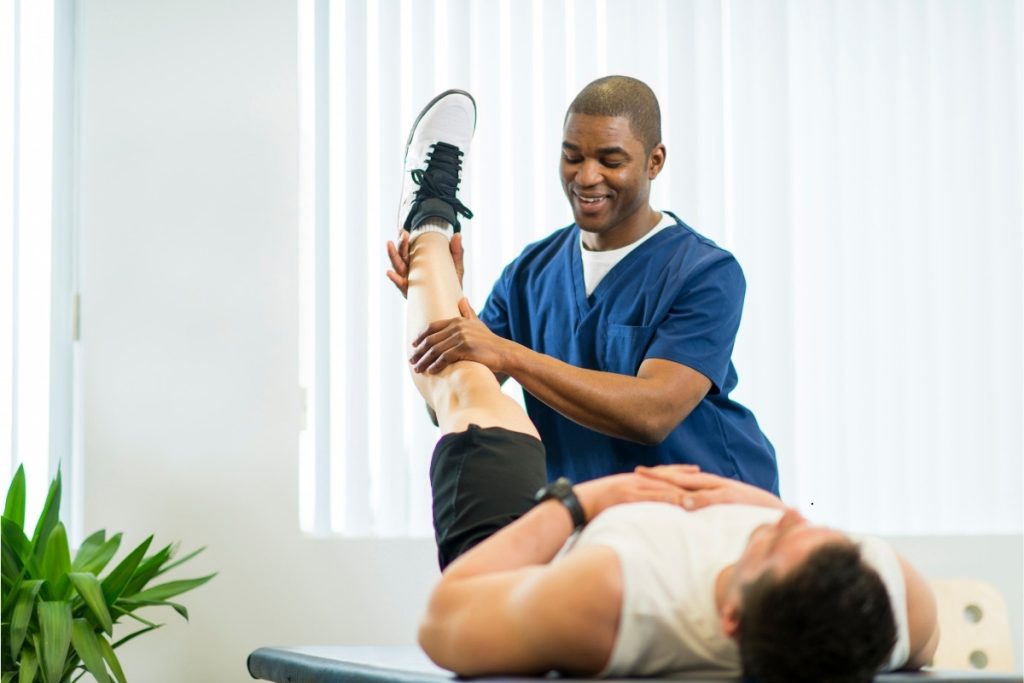
- Targeted physical therapy to restore strength and mobility
- Cortisone or hyaluronic acid injections when appropriate
When symptoms persist or the lesion is unstable, surgery may be considered. Options include:
- Drilling to stimulate blood flow and healing
- Internal fixation to secure a loose fragment
- Cartilage restoration for more advanced cases
If Surgery Becomes the Right Step
Most people do not need surgery. But when surgery is recommended, we explain the reason for it and walk you through the treatment plan in detail.
Before your procedure, you receive a detailed breakdown of:
- Surgical fees and what is included
- Expected insurance coverage
- Facility, anesthesia, and imaging costs
- Estimated out-of-pocket expenses
Post-operative care includes 90 days of structured support, including follow-up visits, recovery care, and any necessary imaging during this period.
What is the Recovery Process for Osteochondritis Dissecans?
Recovery depends on the severity of the condition and how consistently the treatment plan is followed.
- Mild, stable lesions often improve within 3–4 months with rest, activity modification, and physical therapy.
- More advanced cases requiring surgical fixation or cartilage restoration typically take 4–12 months for full recovery.
In both cases, steady rehabilitation helps restore strength and support a safe return to activity.

Why Choose Resilience Orthopedics for Osteochondritis Dissecans Treatment
Every case of osteochondritis dissecans is different, so care should be tailored to your symptoms, imaging, and recovery needs.
At Resilience Orthopedics, you can expect:
- Direct access to care: Schedule a consultation without a referral or insurance approval.
- Thorough evaluation: We carefully review your symptoms and imaging to understand the source of your pain.
- Continuity of care: Dr. Pamela Mehta follows your progress from initial evaluation through recovery.
- Conservative-first approach: Most stable lesions are treated without surgery using structured rehabilitation and activity modification.
- Surgical care when needed: When surgery is recommended, we explain why it’s being considered and what the treatment involves.
Ready to Recover?
Take the first step in getting back to your normal self, and book an appointment with Dr. Mehta today.
We’re ready when you are!
FAQs
Can You Keep Playing Sports With OCD?
It depends on lesion stability. In stable cases, modified low-impact activity may still be possible, while higher-impact sports are usually paused to avoid worsening the condition.
How Long Does Recovery Take?
Mild cases typically improve in 3–4 months with non-surgical care. More advanced cases, especially after surgery, may take 4–12 months for full recovery.
Is Surgery Always Required for Osteochondritis?
No. Many stable lesions heal without surgery, especially in younger patients. Surgery is considered when the lesion is unstable, symptoms persist, or issues such as knee locking occur.
What Exercises are Good for Osteochondral Healing?
Low-impact exercises such as cycling, pool walking, straight leg raises, and isometric quadriceps exercises are typically recommended. High-impact activity, deep squats, and pivoting movements are usually avoided until you are cleared.








